Papilloma in The Mouth: Signs and Prevention


Written and verified by the doctor Maryel Alvarado Nieto
Human papillomaviruses (HPV) are part of the Papillomaviridae family, which is capable of infecting different species. More than 100 types of HPV have been described in humans which affect the skin or mucous membranes. In this article, we’re going to take a closer look at papilloma in the mouth.
The oropharyngeal region is one of the main locations of this virus in the body. In fact, infections of this type have increased in incidence in recent years. What are its main causes? How can you detect it? Find out here!
About the human papillomavirus (HPV)
HPV has been classified into two main groups, depending on the oncogenic capacity of the lesions it produces. High-risk viruses are those involved in the development of cancer.
Meanwhile, low-risk HPV includes viruses that cause lesions considered benign, such as warts or condylomas. Determining the type of virus present in a lesion requires specialized studies.
The causes of papilloma in the mouth
The main source of HPV infection is sexual intercourse. Therefore, it’s classified as a sexually transmitted infection (STI). In fact, it’s the most prevalent viral STI worldwide.
Papilloma in the mouth is less common than in the anogenital region; it results from regular oral sex. In addition, other non-sexual routes of infection are also possible.
In newborns, the birth canal represents the most significant source of infection. Likewise, transplacental passage and passage through amniotic fluid are also a possibility.
On the other hand, autoinoculation, in which a lesion in one body region can serve as a source of infection at a different site, has also been described.

We think you may also enjoy reading this article: The HPV Vaccine and Oral Health: How Are They Related?
Risk factors associated with oral HPV
Several studies have identified some factors that increase the probability of HPV infection. Although the literature is more extensive in relation to anogenital infection, papilloma in the mouth is also related to individual behaviors considered risky.
Apart from oral sex, some of the factors involved in HPV transmission are the following:
- Early initiation of sexual intercourse
- A high number of sexual partners
- Unprotected sexual intercourse
- Smoking
- Habitual alcohol consumption
- A history of infection from other types of HPV
Gender is also listed by some authors as a risk factor, since a higher frequency of oral HPV is observed in men than in women. However, it’s possible that this difference is related to higher consumption of alcohol and tobacco in males, as well as the age of onset of sexual activity.
How does HPV infect humans?
Viral particles need to enter the epithelium in order to infect it. Because of this, it’s been determined that there must be a previous lesion in the skin or mucosa where HPV is going to be located.
However, these wounds are usually microscopic. Thus, any microtrauma can serve as a gateway for the virus to infect. The oral cavity is a region susceptible to this type of trauma.
This need for prior injury is because HPV is only capable of infecting cells in the deepest layer of the squamous epithelium, which is present in the skin and mucosa. Therefore, it’s only possible to observe papilloma in these locations.
The deeper layers provide cells to the outermost layers, as the basal cells reproduce and migrate to the surface. Thus, an HPV-infected cell progresses through the entire thickness of the epithelium.
Clinical manifestations of HPV in the oral cavity
In most cases, HPV infection is asymptomatic and may go unnoticed. However, the lesions it produces have characteristics that allow recognition by dentists and physicians. Its main clinical manifestations are described below.
Oral papilloma
This is small (less than one centimeter in diameter) and usually a single lesion. It’s located on the tongue, soft palate, uvula, frenulum, or vermilion. It has a cauliflower-like appearance, with a pale pink or white coloration.
It’s usually painless and its growth is rapid. It’s caused by strains with low oncogenic risk. It affects people of any age, but is more frequent between 30 and 50 years of age.
Condyloma acuminatum
This lesion is slightly larger than papilloma in the mouth (up to 3 centimeters). It has a cauliflower-like appearance and can be single or multiple. When the latter occurs, the tendency is to group the lesions together.
Condyloma acuminatum is related to subtypes of low oncogenic risk (HPV-6 and HPV-11), but the transmission of this infection occurs sexually.
Multifocal epithelial hyperplasia
In contrast, in multifocal epithelial hyperplasia or Heck’s disease, the lesions are not rough, although they do appear raised. The growth is slow and the coloration is usually the same as that of the location.
They are multiple and usually appear on the lips or on the lateral border of the tongue. It mainly affects children.
Preventing papilloma in the mouth
Since the symptoms can go unnoticed, the prevalence of HPV infection is high, which makes it difficult to take effective measures to avoid infection.
Despite this, the main prevention is based on acquiring responsible sexual behavior. In this regard, sexual education at an early age is fundamental.
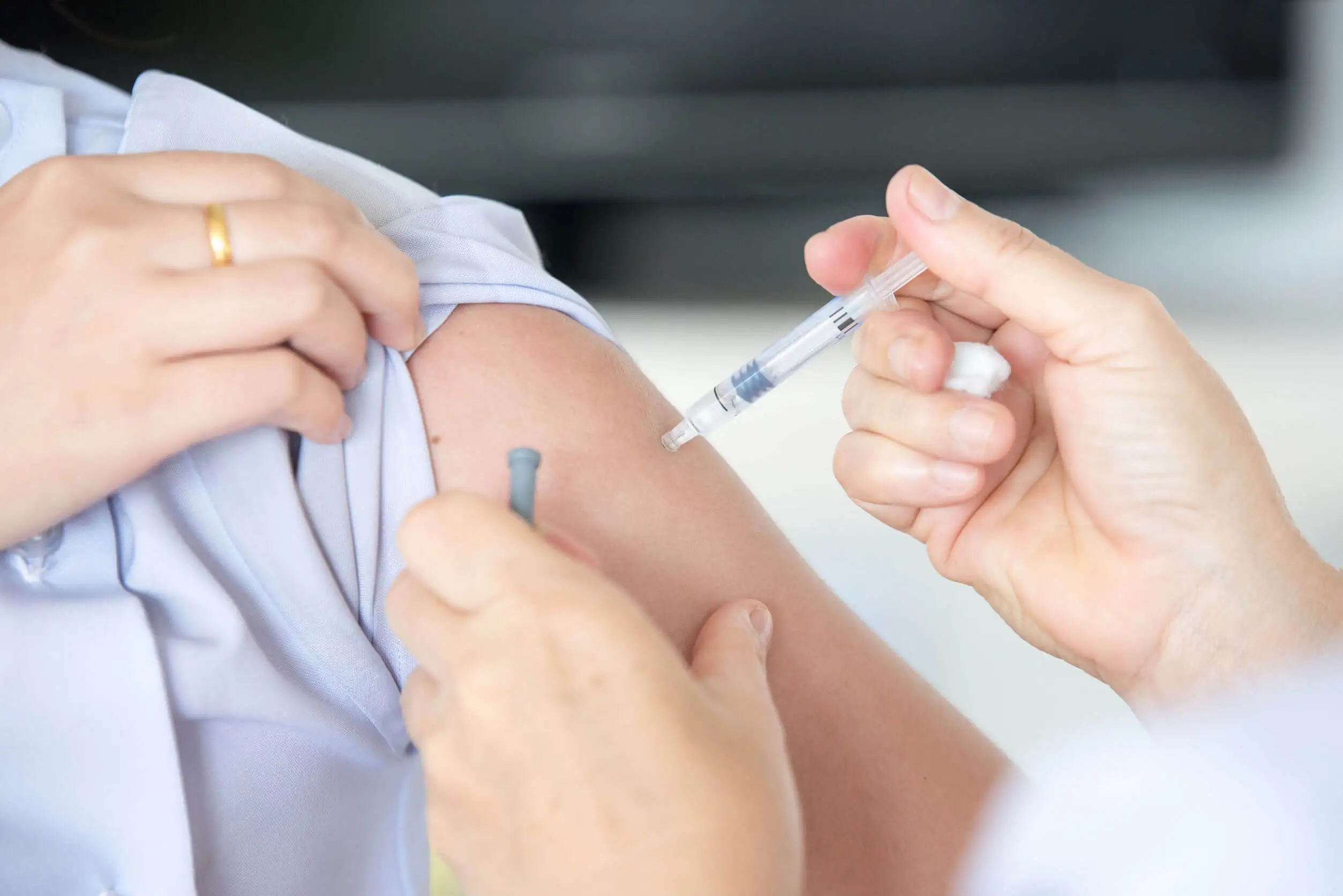
Vaccines and papilloma in the mouth
Vaccines have been designed to prevent infection by some types of HPV, especially those related to the development of cancer. For this reason, the greatest effectiveness in their administration is observed before the onset of sexual life, since the possibility of having been infected prior to the vaccine is negligible.
The current options for HPV prophylaxis are the following:
- Gardasil, manufactured by Merck Laboratories. It protects against HPV types 6, 11, 16, and 18 and is effective in preventing cancer and warts.
- Cervarix, from GlaxoSmithKline. Provides protection against HPV strains 16 and 18, which are involved in the development of cervical neoplasia.
- Gardasil 9, from MSD. It provides immunity against types 6, 11, 16, 18, 31, 33, 45, 52 and 58.
Like this article? You may also like to read: World Immunization Week 2023: The Big Catch Up
Relationship between HPV and oropharyngeal cancer
HPV is the main risk factor for cervical cancer. However, it’s also implicated in neoplasms of the anogenital region and the oropharyngeal cavity.
Of the oncogenic HPV types present in squamous cell carcinoma of the head and neck, HPV 16 is the most frequent. However, unlike cervical cancer, more studies are needed in the oropharynx to establish the characteristics of this region.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Candotto V, Lauritano D, Nardone M, et al. HPV infection in the oral cavity: epidemiology, clinical manifestations and relationship with oral cancer. Oral Implantol (Rome). 2017;10(3):209-220. Published 2017 Nov 30. doi:10.11138/orl/2017.10.3.209
- Contretas, W.; Venegas, L.; Virus Papiloma Humano en Cáncer Oral y Orofaríngeo. Revisión de la Literatura; International Journal of Odontostomatology; 9 (3): 427 -435; 2015.
- Mirghani, H.; Saint-Guily, L.; Virus del Papiloma Humano y Cáncer de Orofaringe; EMC – Otorrinolaringología; 45 (1); 2016.
- Boguñá, N.; Capdevila, L.; Jané-Salas, E.; El Virus del Papiloma Humano y su Relación con la Patología de la Cavidad Oral; Med Clin (Barc); 153 (4): 157 – 164; 2019.
- Cab, B; Hernández, S.; Rueda, F.; Conde, L.; Gómez, J.; Refugio, M.; Epidemiología de la Infección Oral por VPH en Sujetos Jóvenes Sanos; Revista Chilena de Infectología; 34 (6); 557 – 562; 2017.
- Cháirez, P.; Vega, M.; Zambrano, G.; García, A.; Maya, I.; Cuevas, J.; Presencia del Virus Papiloma Humano en la Cavidad Oral. Revisión y Actualización de la Literatura: International Journal of Odontostomatology; 9 (2): 233 -238; 2015.
- Medina, M.; Medina, M; Merino, L.; Consideraciones Actuales sobre la Presencia de Papilomavirus Humano en la Cavidad Oral; Avances en Odontoestomatología; 26 (2); 2010.
- Ledesma, C.; Vega, E.; Garcés M.; Cardiel M.; Juárez C.; Hiperplasia Multifocal del Epitelio. Reporte de Nueve Casos; Medicina Oral Patología Oral y Cirugía Bucal; 10: 394 – 401; 2005.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








