Meningeal Syndrome


Written and verified by the doctor Leonardo Biolatto
Meningeal syndrome isn’t a disease in itself, but a combination of symptoms that indicate the existence of some pathological process in the meninges. The causes can be varied, but, as a general rule, we must say that they always require immediate action.
In medicine, specialists speak of a “syndrome” when a group of signs and symptoms appear together, and when these symptoms could be due to various etiologies. This means that a syndrome can have different diseases as their origin.
In the meningeal syndrome, these three phenomena constitute the set of basic symptoms:
- Cephalea: headache
- Muscle stiffness: due to muscle contractures
- Fever: which may or may not be present, depending on whether the source is infectious or not
The symptoms are evident in a patient when the meninges are already inflamed. The meninges are three very fine, thin layers that cover the inside of the skull and the spine – the structures of the central nervous system. They wrap around the brain and spinal cord as if they were made of paper.
There are three meninges and they’re called dura mater, pia mater and arachnoid. Meningeal syndrome refers to the inflammation of the last two, which the anatomy describes as “leptomeninges”. When these layers become inflamed, they irritate the central nervous system.
Causes of meningeal syndrome
Although there are several causes of meningeal syndrome, the most important are divided into two groups: inflammatory and non-inflammatory. This general division doesn’t determine the severity of the clinical picture, as we’ll explain below.
Keep reading: Sore Throat Relief Options
Inflammatory causes
Within the inflammatory causes we can name:
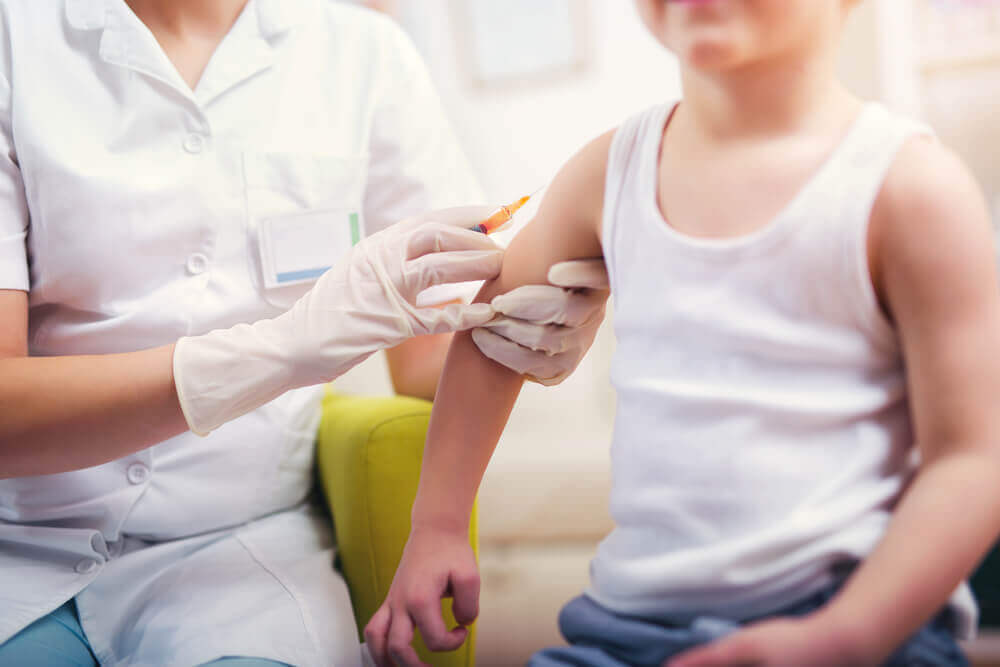
- Bacteria: Perhaps the most important and well-known is meningococcus, a microorganism for which there’s a specific vaccination that can prevent the meningitis it causes. Once the bacterium has settled in, meningeal syndrome is usually complete, and all the symptoms are present. It can also produce outbreaks or epidemics in populations that maintain contact, which is why doctors take extreme precautionary measures when they detect and confirm a case.
- Viruses: Viral meningoencephalitis has a more insidious clinical presentation and includes from relatively common viruses to rare microorganisms that cause specific diseases.
- Fungi: the meningeal syndrome of mycotic cause is rare, but very aggressive. It usually appears in people who have an immunological deficiency and, due to their weakened defenses, are more prone to having the fungi settle in their body. Treatment is also more complicated.
- Parasites: Parasitic meningitis is even rarer and there are only three microorganisms behind almost all cases. Transmission occurs from animals to people, and so the risk is greater in rural workers.
Non-inflammatory causes
The other group of causes are non-inflammatory. Among them:
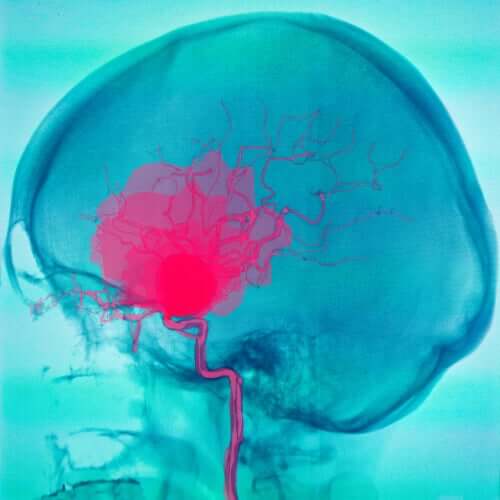
- Hemorrhages: When a stroke occurs because of an artery rupturing in the brain, the hemorrhage forms a collection of blood that, if located near the meninges, inflames them. The result is meningeal syndrome. When the symptoms start, a stroke can be confused with bacterial meningitis, also because of the patient having a fever.
- Traumas: Head traumas, due to blows or accidents can swell the meninges. Various traumatic mechanisms can cause an accumulation of inflammatory fluid between the brain and the leptomeninges, irritating them.
- Neoplasms: Many tumors of the brain, cerebellum, and bone marrow don’t start with more evident signs than those of a meningeal syndrome. The malignant mass that takes place pushes the meninges and ends up irritating them, sometimes without pressing on other structures.
You may want to read: First Aid for Strokes
How to recognize meningeal syndrome
As patients don’t always have a fever with meningeal syndrome, there are two symptoms that are considered key: headache and muscle contractures.
The headaches in these cases are pains that tend to be intense and persistent. The patient often feels the need to yell and shout because of the pain they feel in their skull. The predominant location is the frontal and the occipital one, that’s to say, near the forehead or near the nape of the neck.
This headache usually gets worse and intensifies before stimuli like light or noises. When it intensifies with light, it’s called photophobia, and the patient often has to close their eyes. However, when the pain is worse with sounds, then it’s called algoacusia.
The other characteristic are muscular contractions. In meningeal syndrome, the muscles of the nape of the neck, those of the back and those of the inferior members are often tense and stiff. The stiffness of the nape of the neck doesn’t let the patient move their chin to their chest, for example.
When this stiffness is in the back, then they won’t be able to move their knees to their chest. These have been historical and classic signs that medicine has been associating with meningitis for decades.
Conclusions
If you, or anyone you know, has these symptoms, then visit your doctor right away. The professional will request the necessary studies, usually blood tests and images of the nervous system. They may also resort to a lumbar puncture to study the cerebrospinal fluid if they consider it necessary. Patients and doctors should take these symptoms very seriously as the patient could be very much at risk.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Goic, A., Chamorro, G., Reyes, H.; Semiología Médica; 2010; 3º Edición, Editorial Mediterráneo.
- Leal, MC Rodríguez, et al. “Protocolo diagnóstico y tratamiento empírico del síndrome meníngeo agudo febril.” Medicine-Programa de Formación Médica Continuada Acreditado 12.54 (2018): 3222-3225.
- Weiss, N. “Síndrome confusional y coma.” EMC-Tratado de Medicina 15.1 (2011): 1-8.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








