Dermatofibroma: What Is It Exactly?


Written and verified by the dermatologist Maria del Carmen Hernandez
Dermatofibroma, also called histiocytoma, is a benign tumor that occurs more commonly than you’d think. This doesn’t happen to every single person out there but, perhaps, you’ve been one to notice a small brownish bump on your arms or legs, quite similar to a scar, a nevus, or an ingrown hair.
These lesions, commonly known as dermatofibroma, arise from the accumulation of collagen in the skin. In this article, we’ll be telling you why they occur, how to recognize them, and what therapeutic options there are to control them.
Why does a dermatofibroma appear?
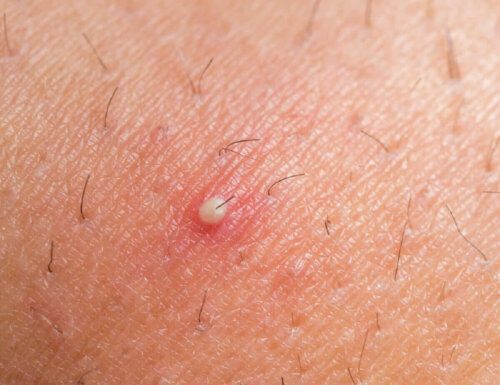
As of now, there’s no exact evidence of the causes of dermatofibroma. However, it’s frequently linked to insect bites, small wounds, pinpricks, or ingrown hairs.
Women are more likely to suffer from this condition than men. On the other hand, a piece of research established that the prevalence of this condition in adults is between the second and fourth decade of life.
Symptoms
In most cases, they don’t cause discomfort. Nonetheless, on rare occasions, they do cause slight pain, especially when compressed. We must mention that it’s very important to consult a specialist whenever there’s new growth on the skin. Let’s see some of the characteristics of dermatofibroma.
- Their color is usually reddish-brown. They can vary in color over time and it’s important to mention that they tend to be darker in people with dark skin.
- They usually appear on the legs, but can also show on the trunk or arms.
- They’re small (less than 1 centimeter – 0.4 in).
- Most of the time, they’re hard to the touch.
- They grow slowly.
- Sometimes they cause itching or tenderness to the touch.
- They’re raised and can bleed if injured.
In immunodeficient patients (transplant recipients, those with HIV, etc.), a large number of dermatofibromas can appear suddenly. People often confuse them with cysts, scars, and moles.
Diagnosing dermatofibroma
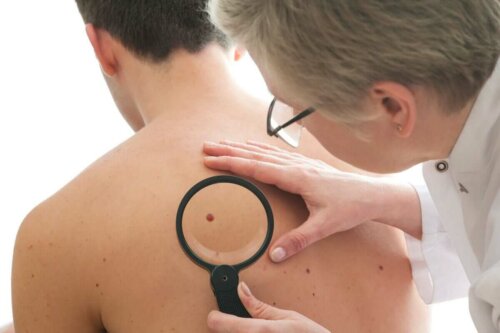
The diagnosis of dermatofibroma is made in the medical consultation through correct questioning. The specialist will ask the patient all about previous injuries in the area. In addition, they’ll ask about the symptoms and do a checkup through touch. After doing this, they’ll be able to determine if this problem truly exists.
Compressing the sides of the lesion produces a characteristic dimple. If the diagnosis isn’t certain, the doctor may turn to dermoscopy or may remove it surgically in order to examine it under a microscope.
Differential diagnostics
Now, there are several pathologies that present similar clinical characteristics to those of dermatofibroma. This is something that the medical professional always needs to bear in mind when making a differential diagnosis. For example, dermatofibrosarcoma protuberans, which refers to a malignant variety of this tumor.
Differential diagnoses include the following:
- Hypertrophic or keloid scar
- Nodular prurigo
- Blue nevus
- Keratoacanthoma
- Juvenile xanthogranuloma
Read also: How to treat keloid scars naturally
The prognosis of dermatofibroma
Dermatofibroma is usually benign, rarely ever do they tend to metastasize. Therefore, any recurrent injury must be followed carefully to get rid of any possible malignancy. On very few occasions, these tumors resolve spontaneously. In addition, they leave areas of post-inflammatory hypopigmentation.
The treatment options for dermatofibroma
This skin lesion doesn’t go away by itself all of a sudden. Despite this, it doesn’t really require specific treatment since it’s not considered a health risk. The only ones that are usually treated are those that generate some aesthetic discomfort or any symptoms, such as pain or itching. Let’s see some of the main treatments for this condition.
Surgical removal
Dermatofibromas are usually pretty deep in the skin. For that reason, removing it through surgery will always leave a small scar. Most doctors choose local anesthesia to perform this. In about 10% of cases, the lesion can arise one more time.
Cryosurgery
Liquid nitrogen freezing is the most widely used treatment. According to a study published in the McGill Journal of Medicine, it reduces or destroys the induration of the tumor and causes a lightening in its color (although not in all cases).
CO2 laser
People get the most satisfactory results through CO2 laser vaporization. However, sometimes the scar is hyperpigmented due to the deep location of the lesion.
CO2 laser is widely used in the field of aesthetic medicine for the treatment of wrinkles and some signs of photoaging. By emitting a specific wavelength, it destroys some of the layers of the skin.
This procedure is easy to tolerate. However, it does have an adverse effect: it can cause redness in the area that’s being treated.
How often do you have to get it checked?
It’s not necessary to carry out a periodic control with a dermatologist since it’s a benign tumor. In case the lesion is irregular, then it’s necessary to get check-ups. This can include the following:
- Poorly defined edges
- Rapid growth
- Reappearance after surgical removal
- Increased depth
If the dermatologist suspects another condition, additional tests will be necessary. In all other cases, no treatment is required beyond aesthetic preferences.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Skin Disease: Diagnosis & Treatment. (3rd Ed), Pag. 436, Thomas P. Habif, James L. Campbell Jr, M. Shane Chapman, James G. H. Dinulos, Kathryn A. Zug.
-
Parish LC, Yazdanian S, Lambert WC, Lambert PC. Dermatofibroma: a curious tumor. Skinmed. 2012;10(5):268-270.
- Clinical Dermatology. Carol Soutor & Maria Hordinsky, (1st Ed) 2013
- Enzinger FM, Weiss SW. Benign fibrohistiocytic tumors. Cap.
13. - McNutt NS, Reed JA. Tumors of the fibrous tissue. Cap 37
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








