Degenerative Joint Disease: Causes and Treatment
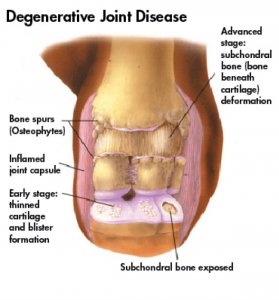
Degenerative joint disease, also known as osteoarthritis, encompasses disorders that affect hyaline cartilage and subchondral bones. It also causes pain, inflammation and prevents normal movements. After all, cartilage is the tissue responsible for covering the ends of these bones and is essential for the proper functioning of the joint.
Degenerative joint disease leads to deterioration of the articular cartilage. Then, the bones begin to wear down and hurt. As the cartilage disappears, the bone reacts and bone tissue forms around the sides causing deformation of the joint.
The Causes of Degenerative Joint Disease
The increase in life expectancy and the aging of the population will make degenerative joint disease the fourth cause of disability by the year 2020. Nobody knows the exact cause yet, but there are some risk factors directly related to its appearance:
- Age. Osteoarthritis increases exponentially from the age of 50.
- Gender. It mainly afflicts women over 50-55 years.
- Genetics. The genetic chance of developing a degenerative joint disease can be up to 65 % when your parents also had it.
- Work activity. Repetitive tasks that involve the joints will lead to joint overload in the long term.
- Extreme physical activity. Athletes are at greater risk of developing osteoarthritis.
- Menopause. The decreases in estrogen levels typical of menopause are high-risk factors for its development.
- Obesity. This doesn’t seem to be a major factor in the development of osteoarthritis. However, the extra weight can certainly aggravate the condition in certain joints, especially in the knees.
- Injuries. Fractures and injuries are a trigger for joint degenerative diseases.
Symptoms
Degenerative joint disease begins gradually. It affects one or several joints and subsequently evolves into morning stiffness that’s usually brief and improves with movement.
As the disease progresses, the mobility of affected joints decreases. It presents as flexion contractures, sensitivity or pain to pressure, and a “cracking” sensation. Sometimes, mechanical blockages also occur as a result of the presence of free bodies inside a damaged joint.
The symptoms of osteoarthritis are varied and progressive. However, the most frequent ones are joint pain, limitation of movements, friction and, in some cases, joint effusion (fluid leakage). Joint pain and inflammation may also appear after long periods of physical inactivity throughout the day. The excess tissue growth of the bone tips that once comprised the joint lead to deformation.
Pain is the symptom that most worries people with osteoarthritis. However, it usually ceases with rest. Nevertheless, as the condition progresses, it may become painful both when moving and resting.
You may also be interested: Treatment to Strengthen Bones and Joints
The Treatment for Degenerative Joint Disease

The first step for treating this condition is to avoid anything that contributes to injuring the joints. Also, each person should have a personalized exercise chart adapted to their needs.
Pain increases due to inflammation of the affected area in the most acute phase of this condition. When it happens, there’ll be a need for anti-inflammatories and/or analgesics to reduce swelling in the area and soothe the pain.
Doctors may also prescribe medication to help.
Chondroprotective medications
These types of medications are the only ones specifically designed for the treatment of degenerative joint disease. This is because they act directly on the affected joints.
Not only do they relieve pain and improve mobility, but they can attack the root of the disease. They have components such as chondroitin sulfate, glucosamine sulfate, and hyaluronic acid.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
-
Schinca, N., & Alvarez, J. (2012). artropatía neuropática o Pie de Charcot. TraumaTología Revista Biomedicina |Traumatología.
-
Paz Jiménez, J.; González-Busto Mújica, I.; Paz Aparicio, J. (2002). Artrosis : patogenia y desarrollo. Rev Ortop Traumatol.
-
Wainstein, E. (2014). Patogénesis de la artrosis. Revista Médica Clínica Las Condes. https://doi.org/10.1016/S0716-8640(14)70098-7
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








