Breast Pain and the Menstrual Cycle

Written and verified by the nurse Maria Marin Garcia
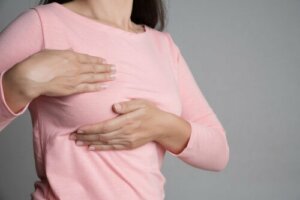
Mastalgia is defined as breast pain. Unfortunately, many women experience it, especially during premenstrual syndrome. Menstruation is influenced by many different factors. In fact, there’s a relationship between breast pain and the menstrual cycle.
It’s common in young women and disappears with the onset of menopause. Approximately 70% of women have experienced it sometime in life. Learn more about this common symptom during menstruation.
What’s the relationship between breast pain and the menstrual cycle?
The menstrual cycle is nothing more than a process that is carried out by the countless hormones that determine how and when the cycle will take place. In this sense, mastalgia is one of the most common symptoms in the different phases of the menstrual cycle.
Usually, it appears during the second half of the cycle (after ovulation, known as the luteal phase) and disappears at the beginning of the menstrual period. During the menstrual cycle, hormonal changes like the following take place:
- Estrogen levels peak at ovulation. This causes a growth of the milk ducts.
- Progesterone peaks a few days later (day 21). This causes an enlargement of the breast lobes, helping cells that are prepared for milk production to form.

To understand it better, the hormonal changes that occur during this phase cause inflammation, swelling, and enlarged breasts, which is painful on many occasions. Also, if the woman becomes pregnant (which keeps progesterone levels high) they’ll stay swollen.
Biologically, the breasts have a greater number of receptors for these substances, which makes them hormone-dependent glands. To a large extent, the breasts react more to hormones than the rest of the body.
You may like this article: Mastalgia: Description and Causes
Causes
Breast pain is mostly related to premenstrual syndrome (the week before menstruation) or benign breast changes (for example, fibrocystic breast disease). Although these are the most common causes, there are some risk factors, such as:
- Following a high-fat diet
- Consuming too much caffeine, theine, or chocolate
- A family history of breast pain during the menstrual cycle
- Certain medications (hormones, antidepressants, etc.)
- Large breast size (increases weight load and may be accompanied by back or neck pain)
Breast pain doesn’t have to be a sign of breast cancer. Only 10% of cases of malignant breast tumors cause mild pain.
Symptoms
There’s a difference between breast symptoms related to the menstrual cycle and those that don’t develop due to cyclical processes.
Breast pain and the menstrual cycle (cyclical)
Breast symptoms influenced by the menstrual cycle are the most common cause of breast pain and are known as premenstrual syndrome. As we already mentioned in this article, they’re caused by hormonal changes that are characterized by the following:
- They affect young women
- As a general rule, they don’t occur during or after menopause
- Homogeneous and bilateral distribution (in other words, both breasts hurt and the pain extends throughout the mammary gland)
- Swelling or inflammation
- Fluid accumulation or retention in the breasts
- Slight increase in breast size
- Turgor (bulging and firm breasts)
- Continuous pain (which can go from mild to severe) only during one stage of the cycle
- To the touch, you feel small lumps throughout the breast
- The symptoms become more intense two weeks before menstruation
- Finally, the pain disappears after menstruation begins
Visit this interesting article: Itchy or Painful Breasts: Treatment and Possible Causes
Non-cyclical breast pain
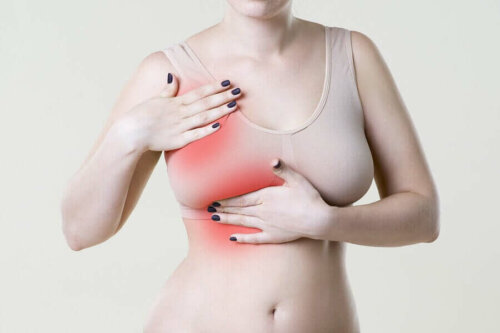
Unlike cyclical pain, other causes can lead to breast symptoms. One of them is usually trauma or benign diseases, such as those we mentioned above. The typical symptoms of non-cyclical breast pain (not common) include the following:
- Continuous or intermittent pain, fixed at one point, described as burning, stabbing, or tearing.
- Inflammation at a certain point of the breast.
- Symptoms don’t vary over time or throughout the menstrual cycle.
- To a greater extent, it occurs after menopause.
- It’s usually unilateral (only one breast hurts).
When to consult a health professional
In general, any non-cyclical cause should be studied. Thus, we recommend you go see a doctor or gynecologist if you suffer from any of them. In addition, you need to be more vigilant if you present any of the following symptoms:
- Change in the shape, color, or appearance of breast skin
- Secretions or fluid in the breasts
- Hormonal changes
- New, unusual, or changing lumps or bumps on the breasts
- Being over 40 and not having had a mammography
- Pain that doesn’t subside and increases in intensity
- Signs of infection (heat, redness, pus, etc.)
- Pain that interferes with daily activity
In short, breast pain is usually associated with the menstrual cycle and the hormonal changes that occur during it. In rare cases, it’s a warning sign of a serious problem. Nevertheless, you need to be alert, especially if the pain is prolonged and severe.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Stanford C hospital. Mastalgia (Breast Pain) [Internet]. [cited 2020 May 6]. Available from: https://www.stanfordchildrens.org/es/topic/default?id=mastalgiabreastpain-85-P03277
- Vendrell E. Dolor mamario. Vol. 3. 1990.
- Mónica Olvera-Mancilla CMO-M. Efectividad del danazol en el control de la mastalgia moderada a severa. 2004.
- Quirino EMB, Pinho CM, Silva MAS, Dourado CARO, Lima MCL de, Andrade MS. Perfil epidemiológico e clínico de casos de microcefalia. Enfermería Glob. 2019 Dec 20;19(1):167–208.
- Yang M, Wallenstein G, Hagan M, Guo A, Chang J, Kornstein S. Burden of premenstrual dysphoric disorder on health-related quality of life. J Women’s Heal. 2008 Jan 1;17(1):113–21.
- Brown J, O’Brien PMS, Marjoribanks J, Wyatt K. Selective serotonin reuptake inhibitors for premenstrual syndrome. In: Cochrane Database of Systematic Reviews. John Wiley & Sons, Ltd; 2002.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








