Birth Control For Skin: Types and Effects


Written and verified by the dermatologist Maria del Carmen Hernandez
Birth control pills are useful for more than just preventing pregnancy and can be effective in treating dermatological issues. They have even been shown to be efficient in correcting some conditions like acne, female pattern hair loss, and hirsutism. Additionally, many women specifically use birth control for skin.
There are different types of birth control pills and they all have both positive and negative effects on the top layers of the skin. This is why we’ll go over some of these issues below. However, you should always speak to your doctor if you have any questions.
What are the side effects of contraceptives?
According to studies by Australian Family Physician, hormonal contraceptives can affect the skin in three different ways:
- Decreasing the amount of androgenic hormones the ovaries and adrenal gland produce.
- Limiting the quantity of testosterone circulating in the bloodstream, and toning down biological activation which is what causes physiological effects.
- Reducing levels of estrogen present in the body, which affects the production of sebum by the sebaceous glands.
Birth control can also have adverse, or negative, effects on the skin. For example, some women experience skin discoloration or hyperpigmentation, an unpleasant reaction that typically occurs after exposure to ultraviolet rays without proper sun protection.
In other words, hormonal contraceptives can cause or worsen melasma, a condition in which dark brown and irregular patches appear in the region above the upper lip, on the forehead, and on the cheeks. A form of this skin condition can occur during pregnancy, which highlights the impact of the hormonal component.
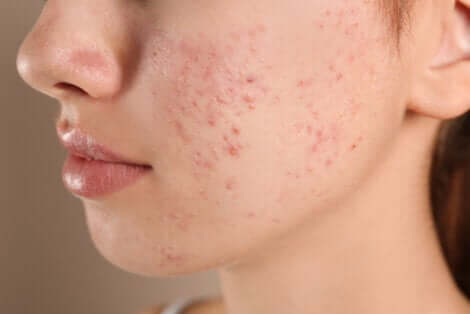
Types of contraceptives and their effects on the skin
Everybody is different, just like hormone levels in each woman are different. With that being said, it’s impossible to predict the side effects someone might have from taking birth control pills. However, there are several types of contraceptives that have been studied extensively and are now common and trusted. Read more about the different types below.
Oral contraceptives
The main reason acne develops during puberty is that the body produces the male sex hormone testosterone in large quantities. Despite its name, both boys and girls produce testosterone.
The use of birth control pills can improve inflammatory acne and non-inflammatory acne. These pharmaceuticals contain the two female sex hormones estrogen and progestin, thus countering androgens.
Despite this, the majority of birth control pills haven’t been specifically approved for treating acne. There are also non-hormonal treatments that can help, some of which have fewer side effects.
Birth control shot
Just one birth control shot can last for up to 90 days. Doctors administer the shot in the deltoid (upper part of the arm) or in the glutes.
Birth control shots, both combined and only with progestin, are a good option for safe, efficient, and reversible contraceptives. Over the years they have gained popularity for their practicality and for saving users from forgetting to take their daily pill, an issue for many women who take the pill.
The birth control shot helps improve acne due to the lowered activity of the sebaceous glands. The explanation is the same as for oral pills.
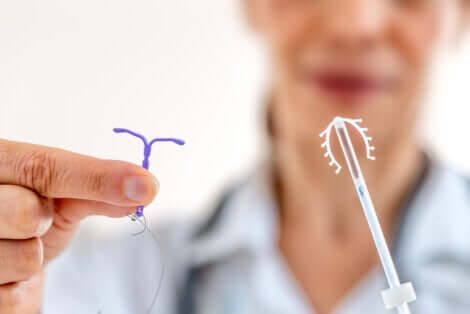
Intrauterine device (IUD)
Copper IUDs are among the contraceptives that don’t contain hormones, similar to condoms, natural birth control methods, and surgery. Thus, copper IUDs don’t affect skin conditions.
On the other hand, hormonal IUDs do give off a limited dose of progestin while placed in the uterus. This, of course, means they’re capable of altering the production of sebum.
Subdermal contraceptive implant
Subdermal contraceptive implants are tiny bars that are injected under the skin, almost always in the upper arm. This contraceptive option continuously releases progestin.
It’s important to mention that progestin’s effects on the skin aren’t as clear as estrogen’s. However, progestin implants lead to an increase in the vasculature as well as an increase in sebum production.
Birth control ring
This contraceptive method is a clear, flexible polyethylene or vinyl acetate ring that, once in the vagina, slowly discharges estrogen hormones and progestin into the body. This way, it prevents the ovaries from releasing eggs during each menstrual cycle.
For people who have used this method of contraception for long periods of time, there has been a notable improvement in acne symptoms. Again, it’s the hormonal component of the contraceptive that’s responsible for this positive effect.
The day-after pill
This type of emergency contraceptive is meant to prevent pregnancy after a woman has had unprotected sex or failed birth control (for example, the condom broke or she missed a pill). The day-after pill is named such because, unlike the other options, it’s supposed to be taken after sex and not before.
Because this pill is high in progestin, its effect is different. It can have androgenic properties as it breaks down in the body, leading to breakouts, and more sebum secretions than usual.
You might like: What Happens if I Vomit After Taking My Birth Control Pill?
Should I use contraceptives for my skin?
According to a study in the Journal of the American Academy of Dermatology, although antibiotics might have better effects on acne after three months of use, oral contraceptives have the same effect after around six months of use. This shows the huge potential contraceptives have in the dermatological industry.
Consequently, taking birth control for skin instead of antibiotics could be the best choice alternative for specifically treating acne in the long term. This could be seen as a secondary advantage to hormonal birth control, in addition to its effects as a method of pregnancy prevention.
If you’re interested in birth control for skin issues you might have, speak with a dermatologist. They’ll help you weigh the risks and determine the level of acne you have in order to identify the best course of treatment.
https://mejorconsalud.as.com/afectan-anticonceptivos-piel/
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Thomas P, Dalle E, Revillon B, Delecour M, Devarenne-nicolle MF, Pagniez I. Bilan cutane de la contraception hormonale [Cutaneous effects in hormonal contraception]. NPN Med. 1985;5(81):19-24.
- Foldes EG. Pharmaceutical effect of contraceptive pills on the skin. Int J Clin Pharmacol Ther Toxicol. 1988;26(7):356-359.
- Effect of contraceptives on the skin. Aust Fam Physician. 1988;17(10):853-856.
- Vaglio, Roxana Fernández, and Natalia Pérez Céspedes. “Acné vulgaris: actualizaciones en fisiopatología y tratamiento.” Revista Ciencia y Salud Integrando conocimientos 4.4 (2020): ág-52.
- Arowojolu AO, Gallo MF, Lopez LM, Grimes DA. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst Rev. 2012;(7):CD004425. Published 2012 Jul 11. doi:10.1002/14651858.CD004425.pub6
- Raudrant D, Rabe T. Progestogens with antiandrogenic properties. Drugs. 2003;63(5):463-492. doi:10.2165/00003495-200363050-00003
- Requena, C., and B. Llombart. “Oral Contraceptives in Dermatology.” Actas Dermo-Sifiliográficas (English Edition) (2020).
- Crimer, Nicole, Roberto Mercau, and David Colica. “Tratamiento del acné en la adolescencia.” Evidencia, actualizacion en la práctica ambulatoria 21.3 (2018).
- Gómez-Flores, Minerva, and Sonia Chávez-Álvarez. “Asociaciones hormonales del acné y su tratamiento.” Dermatología Revista Mexicana 63.S1 (2020): 25-32.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








